What Is Granulation Tissue and Why It Matters for Wound Healing
What Is Granulation Tissue and Why It Matters for Wound Healing

Granulation tissue is a vital component of the wound healing process, characterized by the formation of new connective tissue and microscopic blood vessels. This tissue plays a crucial role in repairing damaged skin and underlying structures, facilitating the transition from inflammation to tissue regeneration. Understanding granulation tissue is essential for anyone involved in wound care, as it not only indicates healing progress but also helps identify potential complications. In this article, we will explore the definition and role of granulation tissue, the formation process during wound healing stages, the cells involved, how to identify healthy versus unhealthy tissue, and best practices for promoting its growth.
What Is Granulation Tissue and What Role Does It Play in Wound Healing?
Granulation tissue is a temporary, new tissue that forms at the site of a wound during the healing process. It consists of a network of collagen fibers, blood vessels, and inflammatory cells, which work together to provide a scaffold for new tissue growth. This tissue is essential for wound healing as it fills the wound bed, supports the migration of epithelial cells, and ultimately leads to the formation of scar tissue. The presence of healthy granulation tissue is a positive sign, indicating that the body is effectively responding to injury and working towards recovery.
How Does Granulation Tissue Form During the Wound Healing Stages?
The formation of granulation tissue occurs in the proliferative phase of wound healing, which follows the inflammatory phase. During this stage, fibroblasts migrate to the wound site and begin synthesizing collagen, which provides structural support. Additionally, angiogenesis, the formation of new blood vessels, occurs to supply oxygen and nutrients to the healing tissue. A moist environment is crucial during this phase, as it promotes cell migration and reduces the risk of infection, facilitating the development of granulation tissue.
Further emphasizing the role of new blood vessel formation, research highlights how angiogenic capillary sprouts are integral to the developing granulation tissue.
Angiogenesis in Granulation Tissue Formation
During wound healing, angiogenic capillary sprouts invade the fibrin/fibronectin-rich wound throughout the granulation tissue.
Angiogenesis in wound healing, X Feng, 2000
Which Cells and Biological Processes Are Involved in Granulation Tissue Development?
Several key cells and biological processes are involved in the development of granulation tissue. Fibroblasts are the primary cells responsible for producing collagen and extracellular matrix components, which are essential for tissue repair. Angiogenesis is driven by growth factors such as vascular endothelial growth factor (VEGF), which stimulates the formation of new blood vessels. Macrophages also play a critical role by clearing debris and releasing cytokines that promote healing. Together, these processes ensure the effective formation of granulation tissue, which is vital for successful wound healing.
The intricate regulation of VEGF-A expression, particularly by factors like hypoxia and HIF-1, is crucial for optimal granulation tissue development.
Hypoxia, HIF-1, and Vegfa in Granulation Tissue Formation
Hypoxia in skin wounds is thought to contribute to healing through the induction of hypoxia inducible factor-1 (HIF-1). Although HIF-1 can regulate the expression of vascular endothelial growth factor A(Vegfa), whether hypoxia and HIF-1 are required to induceVegfaexpression in the context of wound healing is unknown. To test this hypothesis, we evaluatedVegfaexpression and wound healing in mutant mice that lack a functional HIF-1 binding site in theVegfapromoter. Full-thickness excisional wounds were made using a biopsy punch, left to heal by second intention, and granulation tissue isolated on a time course during healing.
A hypoxia response element in the Vegfa promoter is required for basal Vegfa expression in skin and for optimal granulation tissue formation during wound healing …, P Carmeliet, 2017
Beyond its expression, the specific signaling pathways, such as those involving VEGFR1, are also critical in facilitating granulation tissue formation.
VEGFR1 Signaling in Granulation Tissue Formation
Vascular endothelial growth factor (VEGF)-A facilitates wound healing. VEGF-A binds to VEGF receptor 1 (VEGFR1) and VEGFR2 and induces wound healing through the receptor’s tyrosine kinase (TK) domain. However, the precise mechanism of wound healing, especially granulation formation on VEGFR1, is not well understood. We hypothesized that VEGFR1-TK signaling induces wound healing by promoting granulation tissue formation.
Vascular endothelial growth factor receptor 1 (VEGFR1) tyrosine kinase signaling facilitates granulation tissue formation with recruitment of VEGFR1+ cells from bone …, 2018
How Can You Identify Healthy Versus Unhealthy Granulation Tissue?
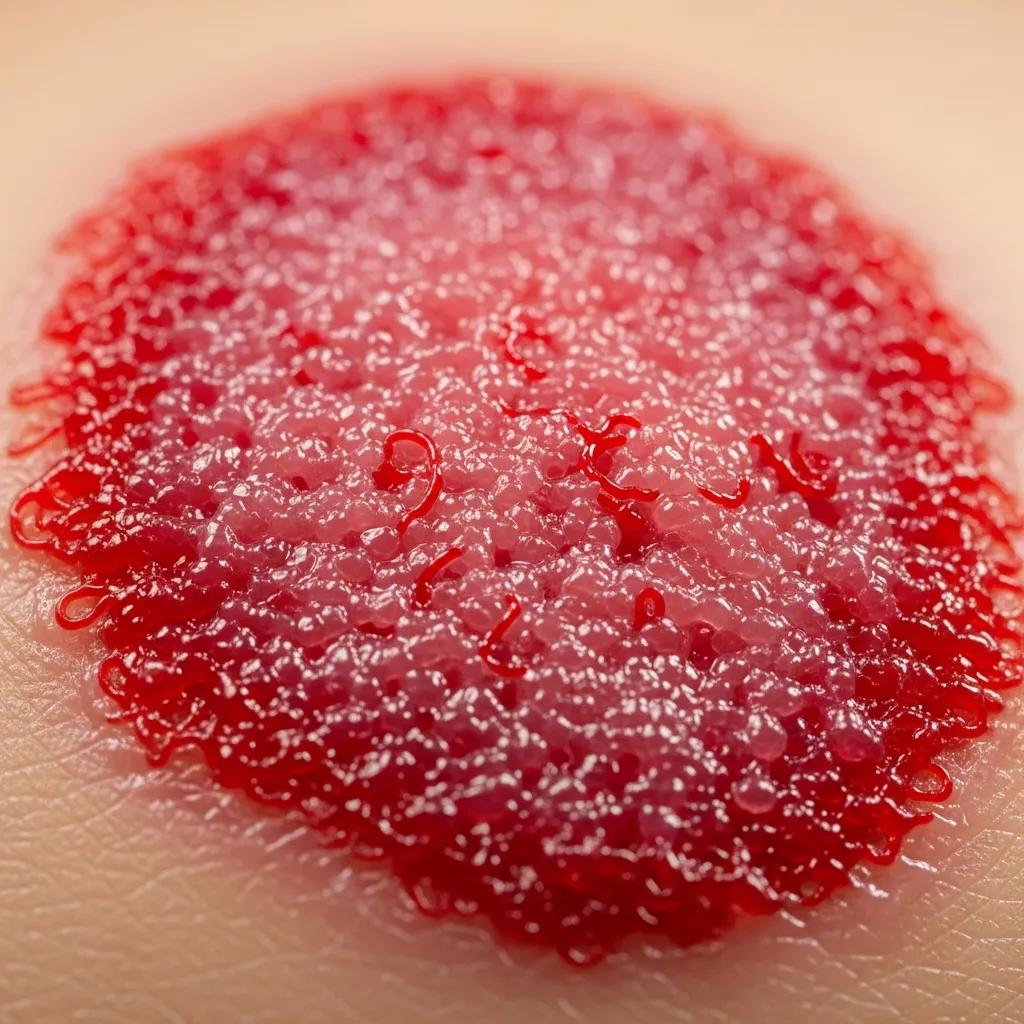
Identifying healthy versus unhealthy granulation tissue is crucial for effective wound management. Healthy granulation tissue typically appears red or pink, is moist, and has a granular texture. In contrast, unhealthy granulation tissue may appear pale, dry, or excessively swollen, indicating potential complications such as infection or poor blood supply. Regular monitoring of the wound and its granulation tissue can help healthcare providers make informed decisions about treatment and intervention.
What Are The Visual Signs of Healthy Granulation Tissue?

Healthy granulation tissue exhibits several visual signs that indicate proper healing. These include:
- Color: Healthy granulation tissue is usually bright red or pink, indicating good blood flow.
- Texture: It has a moist, granular appearance, which is essential for effective healing.
- Size: The tissue should gradually fill the wound bed without excessive growth or necrosis.
Recognizing these signs can help caregivers assess the healing process and determine if further intervention is necessary.
What Complications Arise from Unhealthy or Infected Granulation Tissue?
Unhealthy or infected granulation tissue can lead to several complications that hinder the healing process. Potential issues include:
- Infection: Signs of infection may include increased redness, swelling, and discharge from the wound.
- Delayed Healing: Poorly formed granulation tissue can slow down the overall healing process, leading to chronic wounds.
- Scarring: Inadequate granulation tissue may result in excessive scarring or keloid formation.
Timely intervention and proper wound care management are essential to address these complications and promote healthy granulation tissue development.
What Are Best Practices for Wound Care Management to Promote Granulation Tissue Growth?
Effective wound care management is crucial for promoting the growth of granulation tissue. Best practices include:
- Debridement Techniques: Regularly removing dead tissue and debris from the wound bed helps create an optimal environment for healing.
- Moisture Management: Keeping the wound moist with appropriate dressings can enhance cell migration and granulation tissue formation.
- Nutritional Support: Ensuring adequate nutrition, particularly protein intake, supports the body's healing processes.
Dinkum Prospect Healthcare specializes in delivering personalized wound care services, focusing on these best practices to enhance healing outcomes for patients in the DC Metro area.
Which Wound Care Techniques Support Optimal Granulation Tissue Formation?
Several wound care techniques can support optimal granulation tissue formation, including:
- Negative Pressure Wound Therapy: This technique uses suction to promote blood flow and tissue granulation.
- Advanced Dressing Options: Hydrocolloid and alginate dressings can maintain a moist environment conducive to healing.
- Maintaining a Moist Environment: Keeping the wound hydrated is essential for promoting cell migration and granulation tissue growth.
These techniques are integral to effective wound management and can significantly impact healing outcomes.
When Should Patients Seek Professional Care for Chronic Wounds?
Patients should seek professional care for chronic wounds when they notice:
- Signs of Non-Improvement: If the wound does not show signs of healing after a few weeks, it may require professional assessment.
- Indicators of Infection: Increased pain, redness, or discharge can signal an infection that needs medical attention.
- Persistent Granulation Tissue Issues: If granulation tissue appears unhealthy or excessive, professional evaluation is necessary to determine the best course of action.
Recognizing these signs early can lead to timely interventions and better healing outcomes.